Welcome to the monthly SHDA Research Update. Our specialists have selected 3 seminal papers that have been recently published in each speciality (Cardiology, Cardiac Surgery, Cardiac Imaging, Perioperative Medicine).
Cardiology
Summarised by Dr Sarah Catchpoole
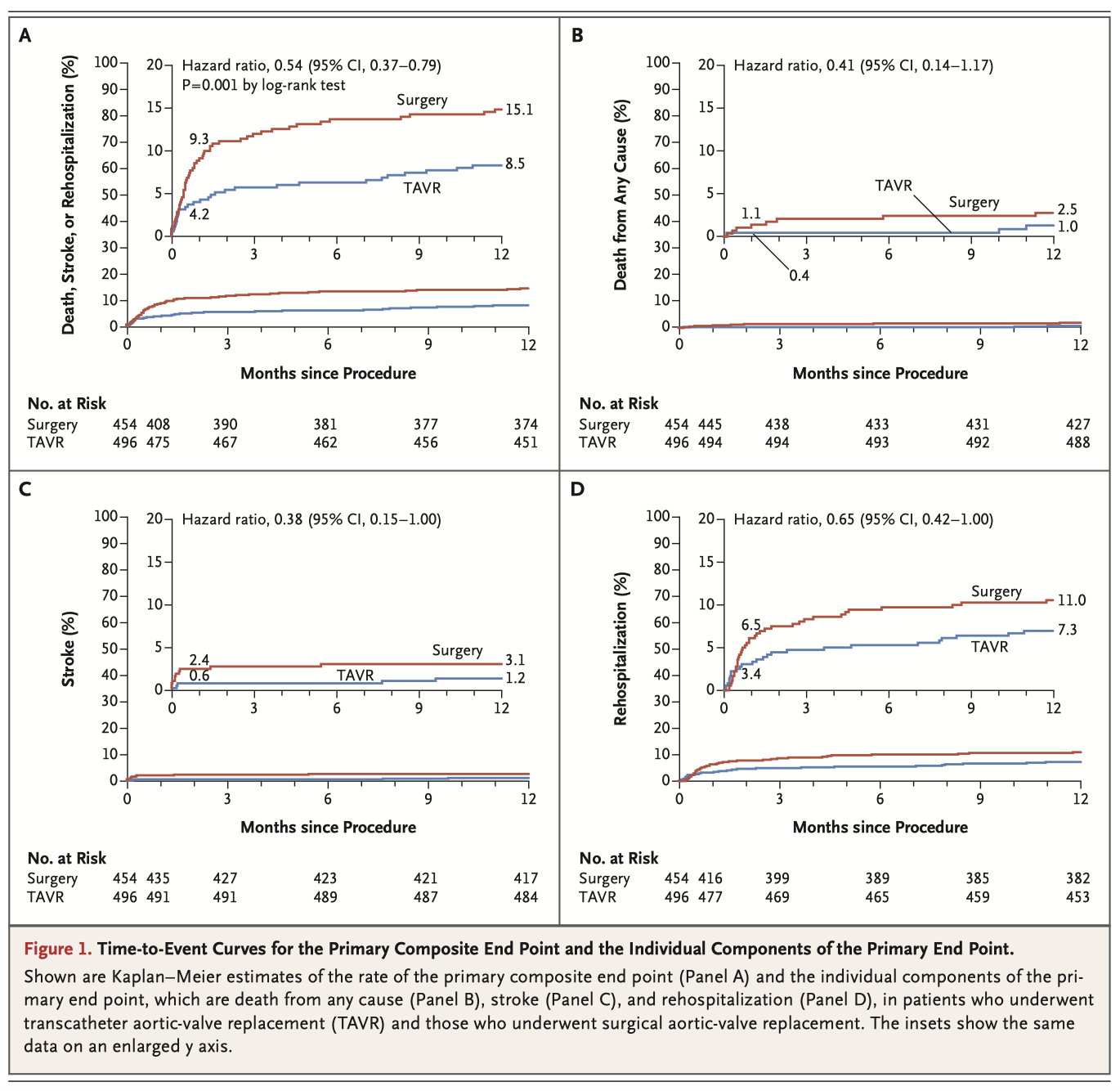
Transcather aortic valve replacement (TAVR), once reserved for those considered high operative risk, is being increasingly explored as an alternative to surgery in lower-risk patient populations. In this randomised control trial, 1000 low-risk patients with severe calcific aortic stenosis were allocated to either TAVR or Surgery across 71 sites. TAVR was superior at both 30 days and 1 year for all three separate components of the primary end point (death, stroke and rehopitalisation) and was overall superior using the composite primary end point at 1 year (8.5% vs. 15.1, P<0.001 for noninferiority, P=0.001 for superiority). In addition, TAVR was associated with better outcomes on multiple secondary end points and resulted in more rapid improvement in functional status.
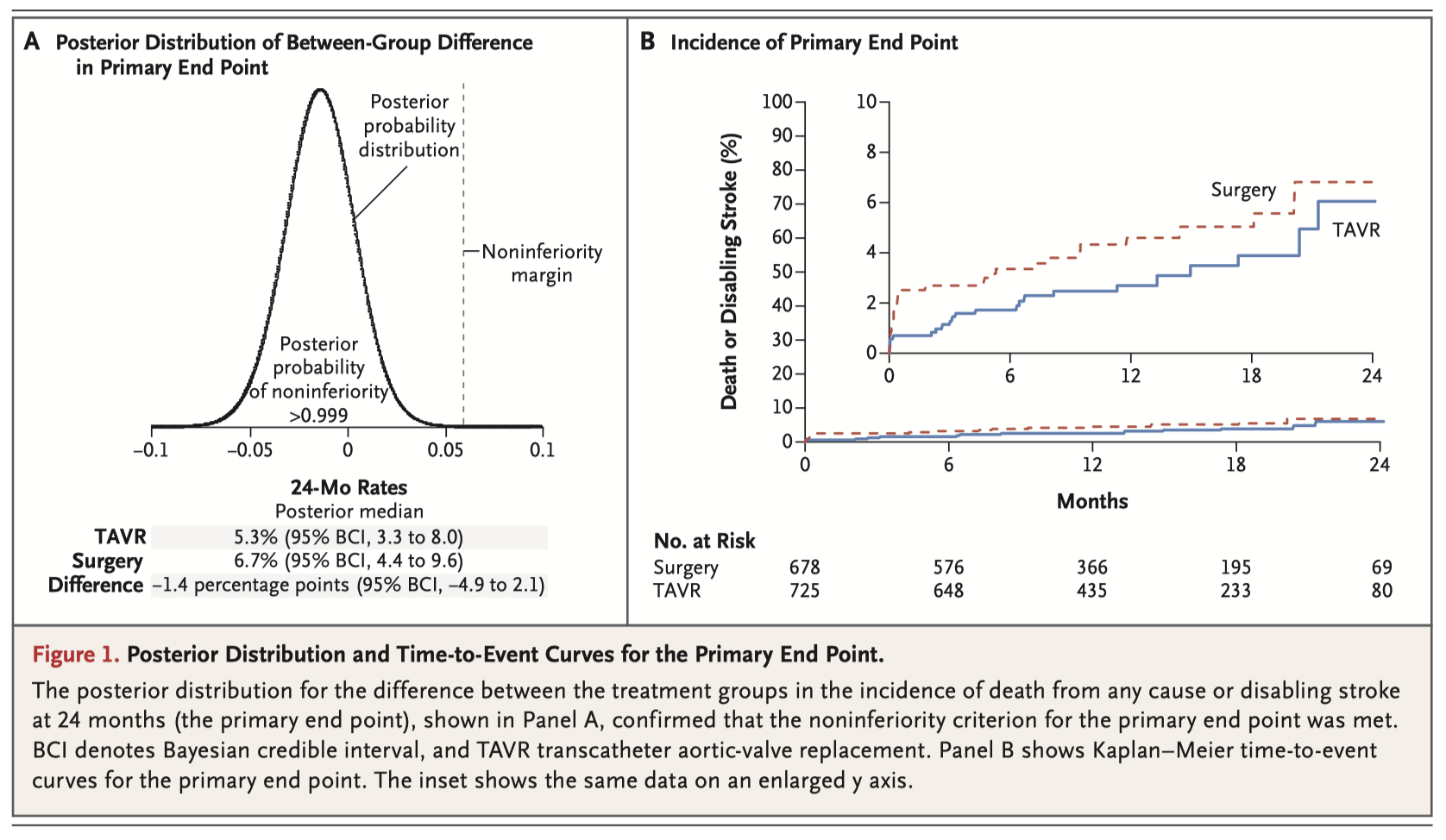
This paper reports the interim results after a median of 12.2 months follow up from a cohort of 1403 low-risk patients with severe aortic stenosis. Patients were randomised to either transcather aortic valve replacement (TAVR, n=725) or surgery (n=678). Using Bayesian methods, the estimated 24-month estimated incidence of the primary end point (death or disabling stroke) was 5.3% in the TAVR group and 6.7% in the surgery group, demonstrating non-inferiority of TAVR compared to surgery. At 30 days, TAVR patients had better early functional outcomes and lower rates of disabling stroke, acute kidney injury, bleeding events and atrial fibrillation; but higher rates of permanent pacemaker insertion and aortic regurgitation.
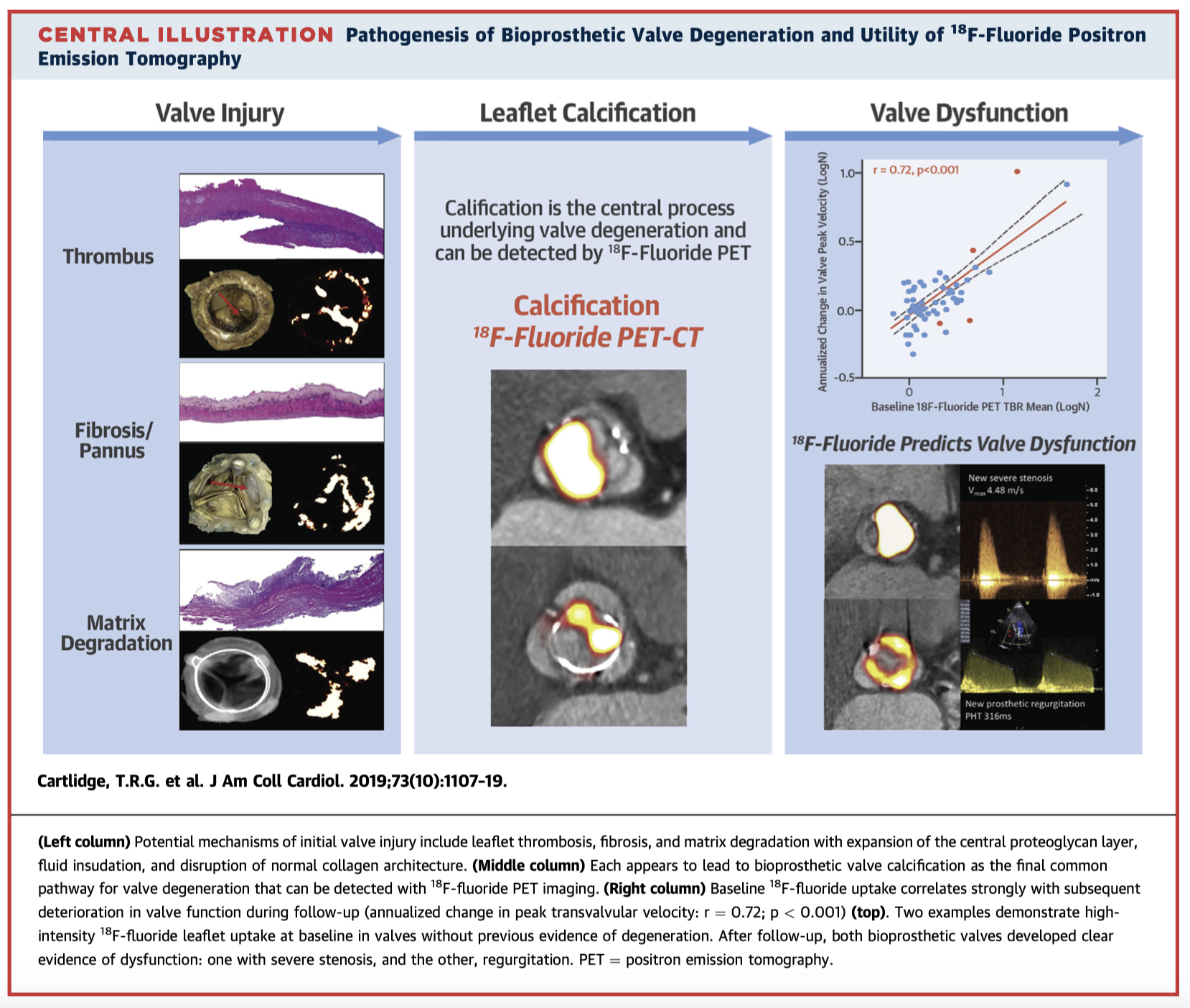
18F-fluoride preferentially binds to areas of developing microcalcification, one of the key pathological processes though to underlie bioprosthetic valve degeneration (see Central Illustration). This study confirms the potential of 18F-fluoride PET-CT for early identification of valve dysfunction. In laboratory studies of failed explanted valves, there was strong correlation between increased fluoride activity and areas of histologic tissue degeneration. Secondly, in a prospective cohort of 71 patients without known valve dysfunction, increased F-flouride uptake was associated with poorer performance on conventional echocardiographic parameters, and was an independent predictor of bioprosthetic valve degeneration.
Cardiac Surgery
Summarised by Dr Andrew Haymet
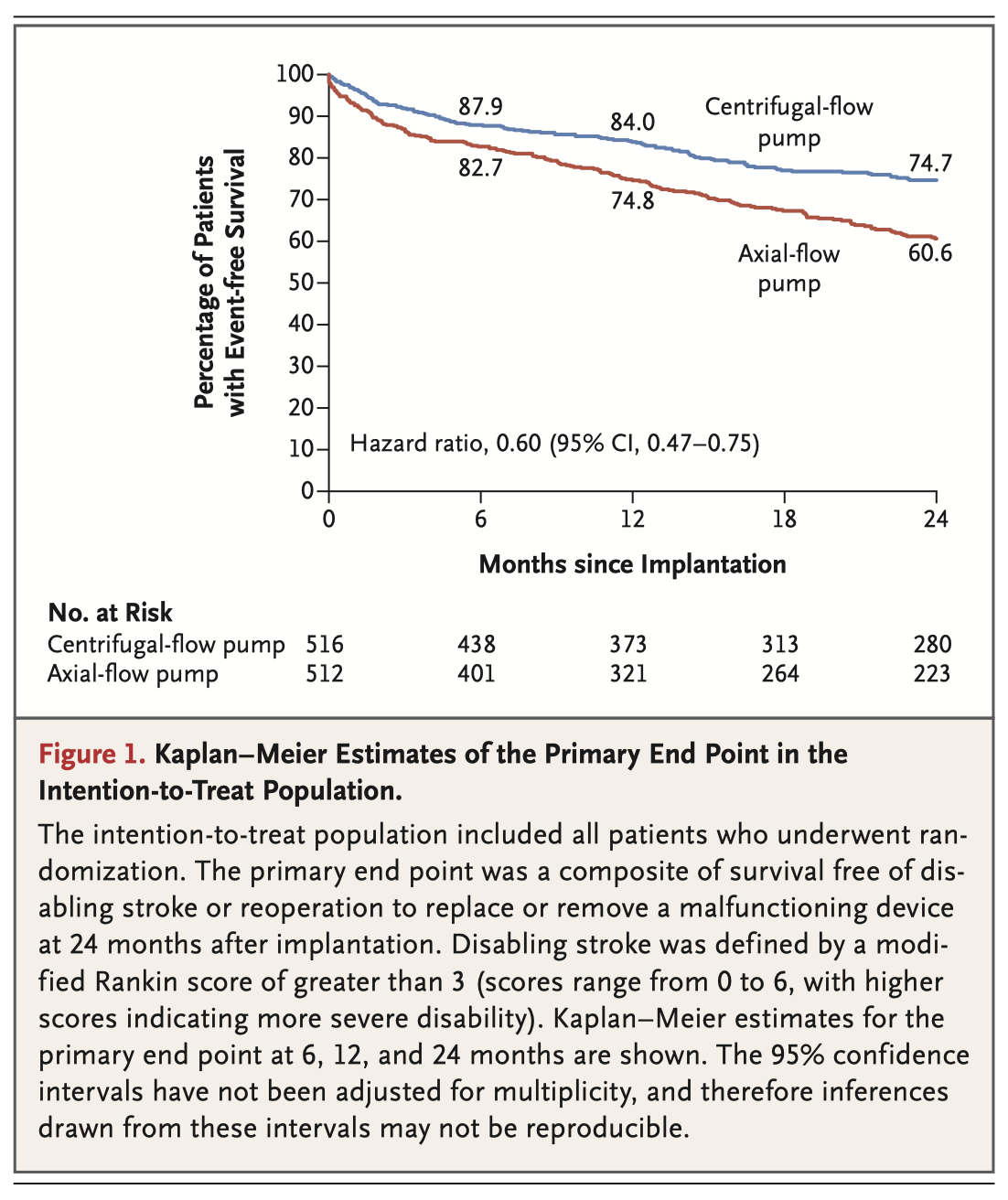
This final analysis of 1028 patients randomly assigned patients with advanced heart failure to receive either the centrifugal-flow pump or the axial-flow pump. The composite primary end point was survival at 2 years free of disabling stroke or reoperation. The authors concluded that a fully magnetically levitated centrifugal flow LVAD was associated with a less frequent need for pump replacement than an axial flow device, and was superior with respect to survival free of disabling stroke or reoperation to replace or remove a malfunctioning device.
This study of 314 patients aimed to describe the procedural and clinical outcomes of patients undergoing transcarotid (TC) transcatheter aortic valve replacement (TAVR) with the Edwards Sapien 3 device. The authors concluded that TC-TAVR using the Edwards Sapien 3 device was safe and effective. The TC approach might be considered, in selected patients, as the first-line alternative approach for TAVR whenever the transfemoral access is prohibited.
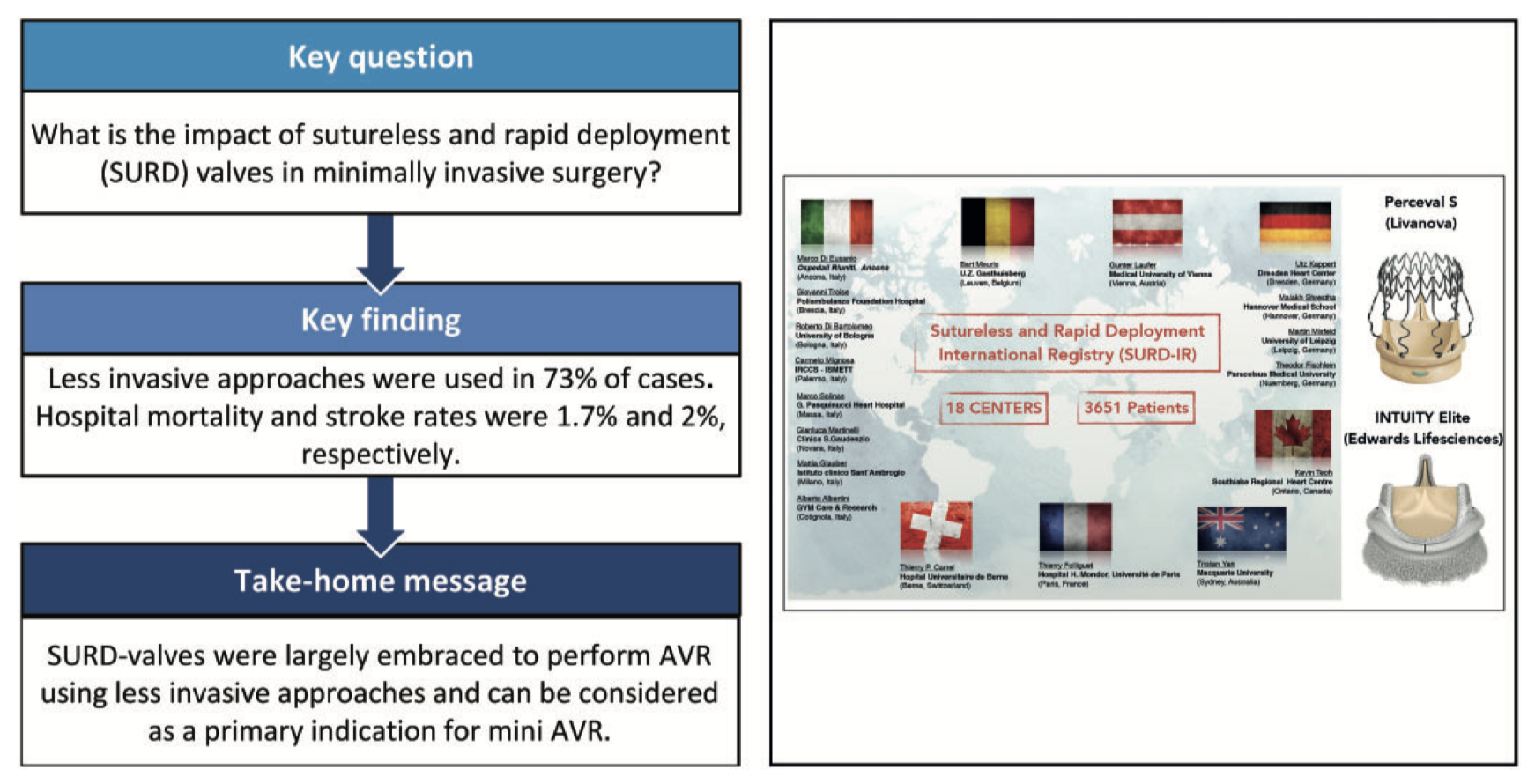
This study of 1935 patients aimed to assess clinical characteristics and in-hospital results of patients receiving sutureless and rapid deployment aortic valve replacement (SURD-AVR) through less invasive approaches in the large population of the Sutureless and Rapid Deployment International Registry (SURD-IR). In the SURD-IR cohort, minimally invasive SURD-AVR using both Perceval and Intuity valves appeared a safe and reproducible procedure associated with promising early results.
Cardiac Imaging
Summarised by Dr Sarah Catchpoole
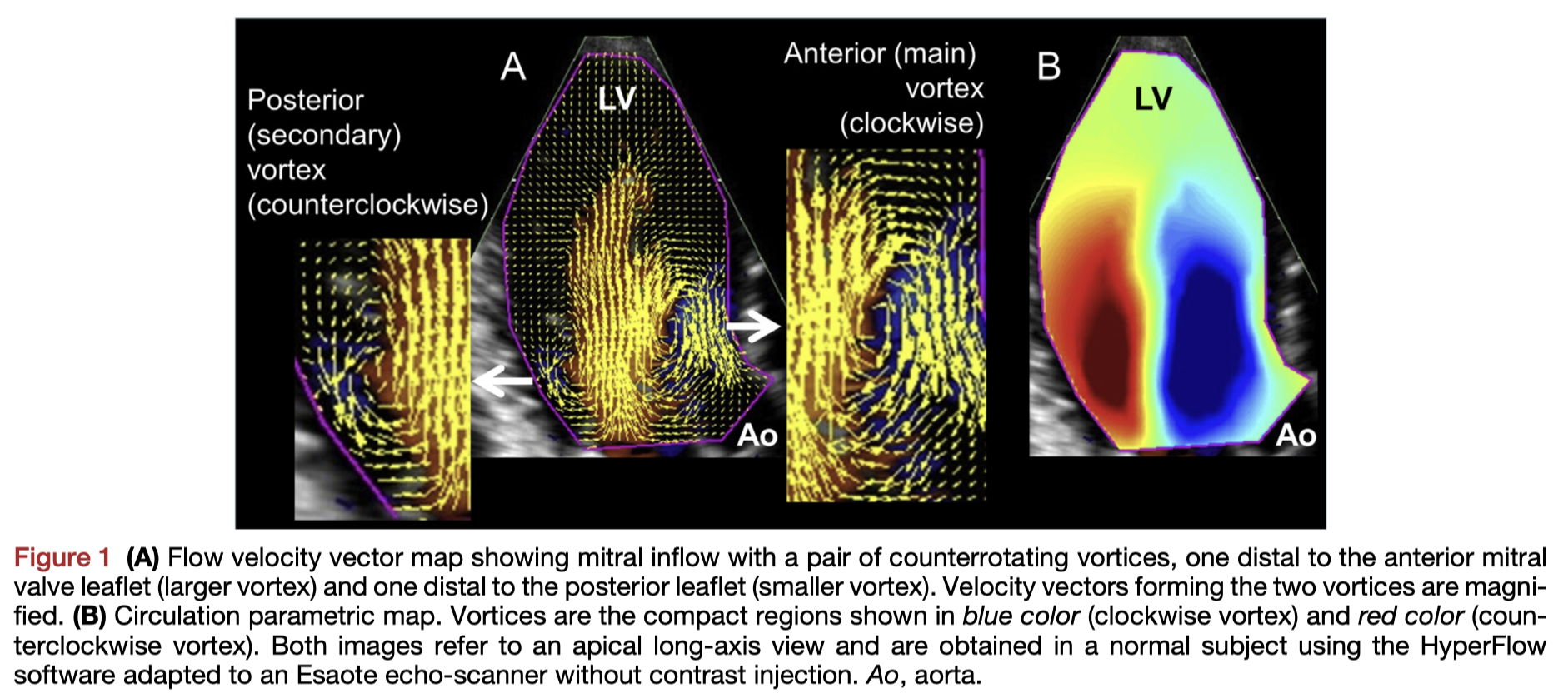
Intra-cardiac flow analysis has contributed significantly to our understanding of cardiac pathophysiology in experimental settings. However, despite improvements in technology permitting examination of flow using non-invasive, non-contrast ultrasound techniques, flow analysis has not entered clinical practice. This review introduces the basic concepts in flow dynamics, vortex behavior, and current available imaging techniques. While validation studies are needed, the review discusses potential clinical applications in specific disease states including structural, ischaemic and arrhythmic cardiac disorders.
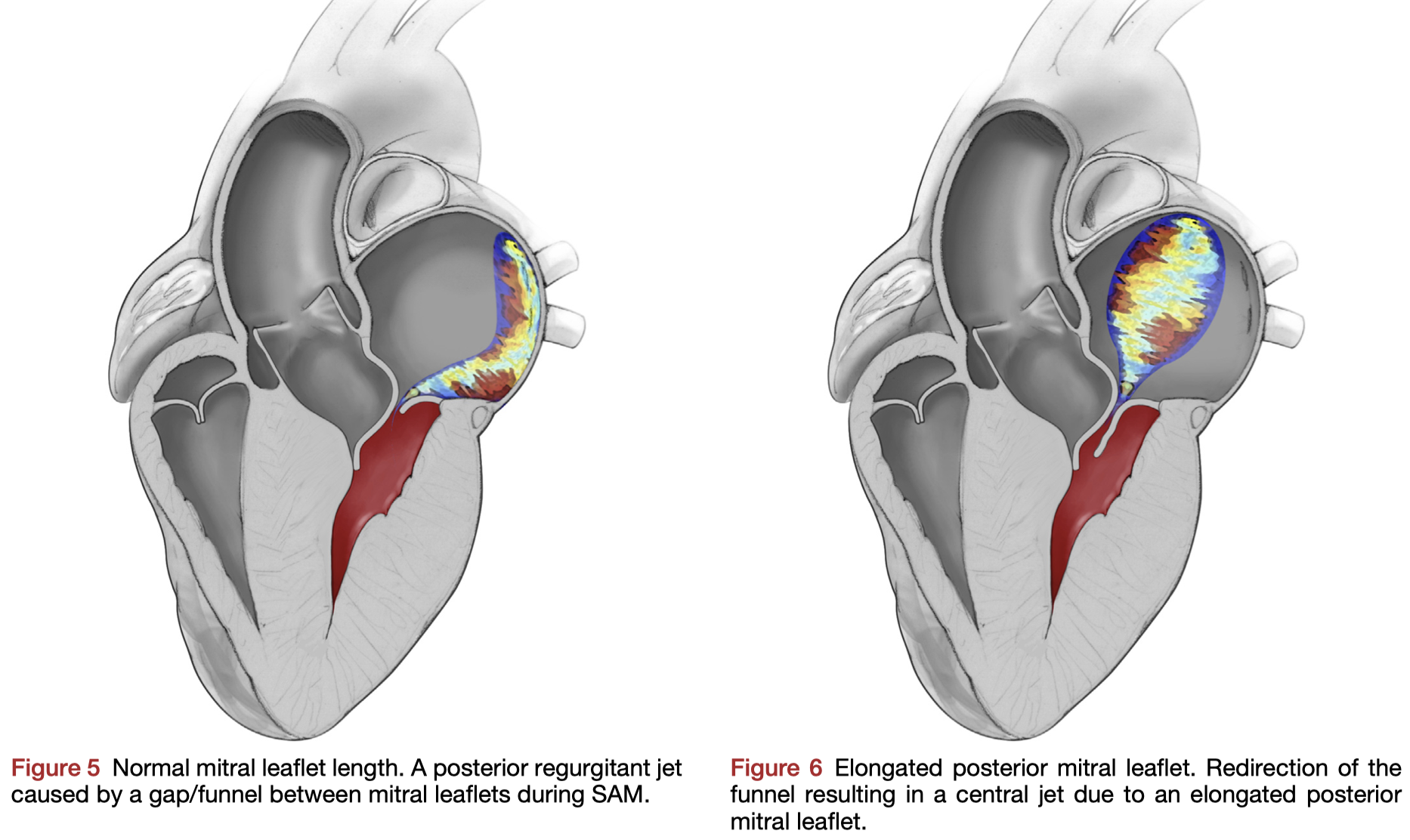
Mitral regurgitation (MR) in hypertrophic cardiomyopathy (HCM) can be divided into (A) native (or intrinsic) mitral valve disease, or (B) MR mediated by abnormal systolic anterior motion (SAM), typically characterized by a posteriorly directed jet on echocardiography. In this study, 330 patients with HCM and MR underwent echocardiographic evaluation both before and after septal myectomy. A posteriorly directed jet had a positive predictive value for SAM mediated MR of 94.9%. However, the negative predictive value was low at 17.4%. The author’s recommend caution when using the jet direction on pre-operative echocardiography in clinical decision making for concurrent mitral valve surgery.
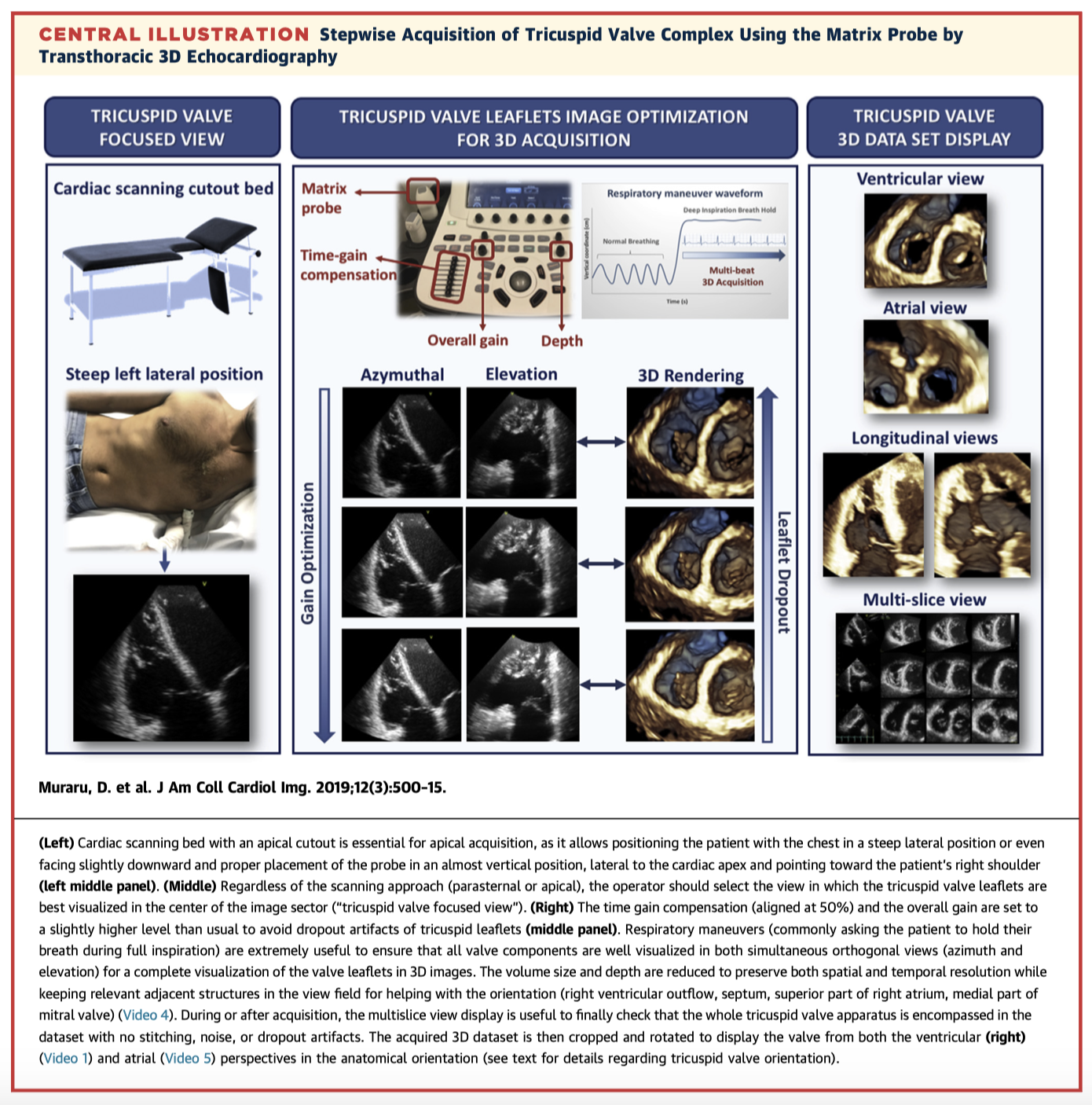
This review provides a comprehensive overview of 3D transthoracic echocardiographic (3D TTE) imaging of the Tricuspid Valve (TV). Given the valve’s anterior location, complex geometry and highly variable anatomy, 3D imaging provides incremental value over conventional 2D echocardiography and is now an essential and cost-effective way to better defines the TV complex for functional assessment and peri-procedural planning.
Perioperative Medicine
Summarised by Dr Andrew Haymet
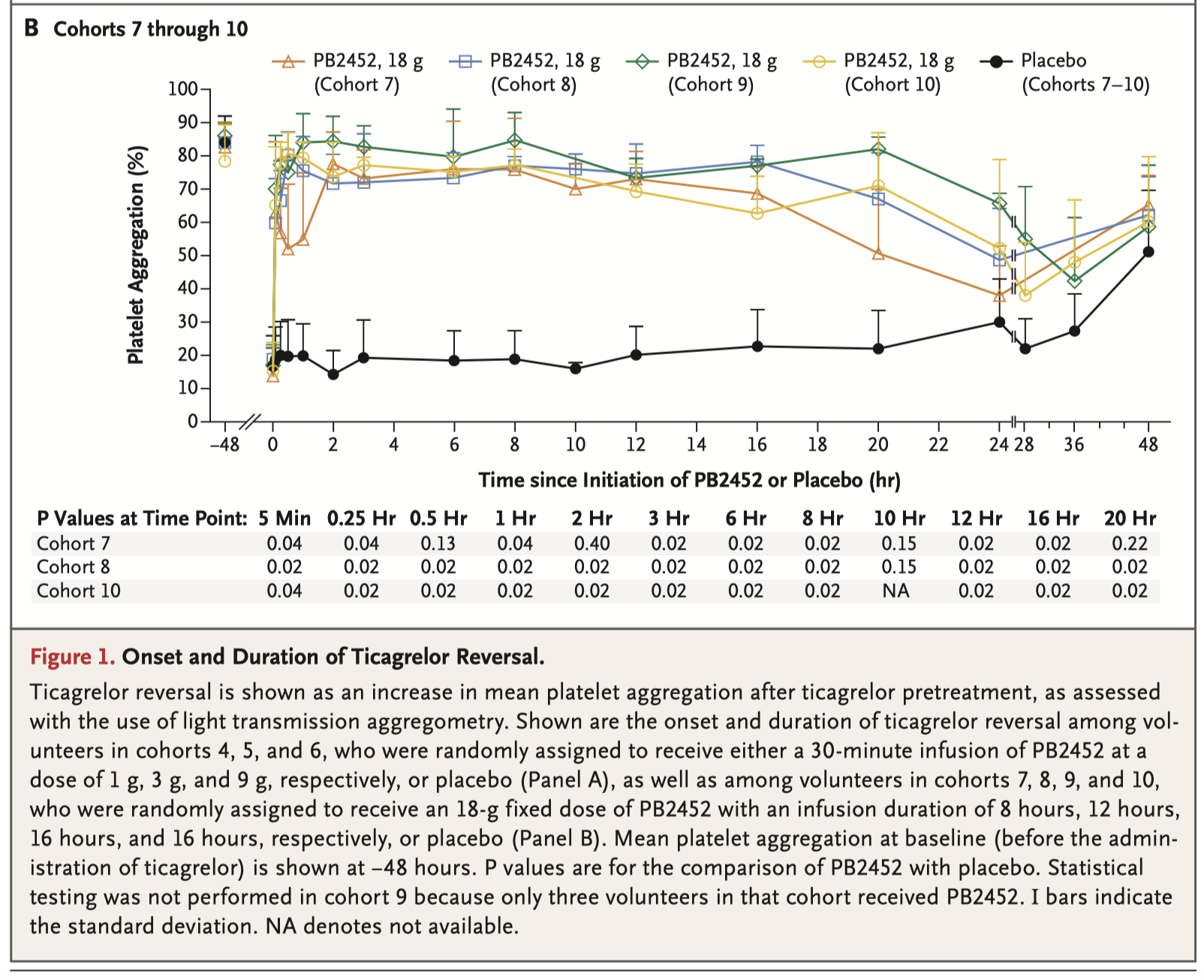
Ticagrelor is an oral P2Y inhibitor that is used with aspirin to reduce the risk of ischaemic events among patients with acute coronary syndromes or previous myocardial infarction. This randomized phase 1 trial of 64 volunteers evaluated PB2452, a monoclonal antibody fragment that binds ticagrelor with high affinity as a reversal agent. The authors concluded that in healthy volunteers, PB2452 provided immediate and sustained reversal of the antiplatelet effects of ticagrelor, as measured by multiple assays.
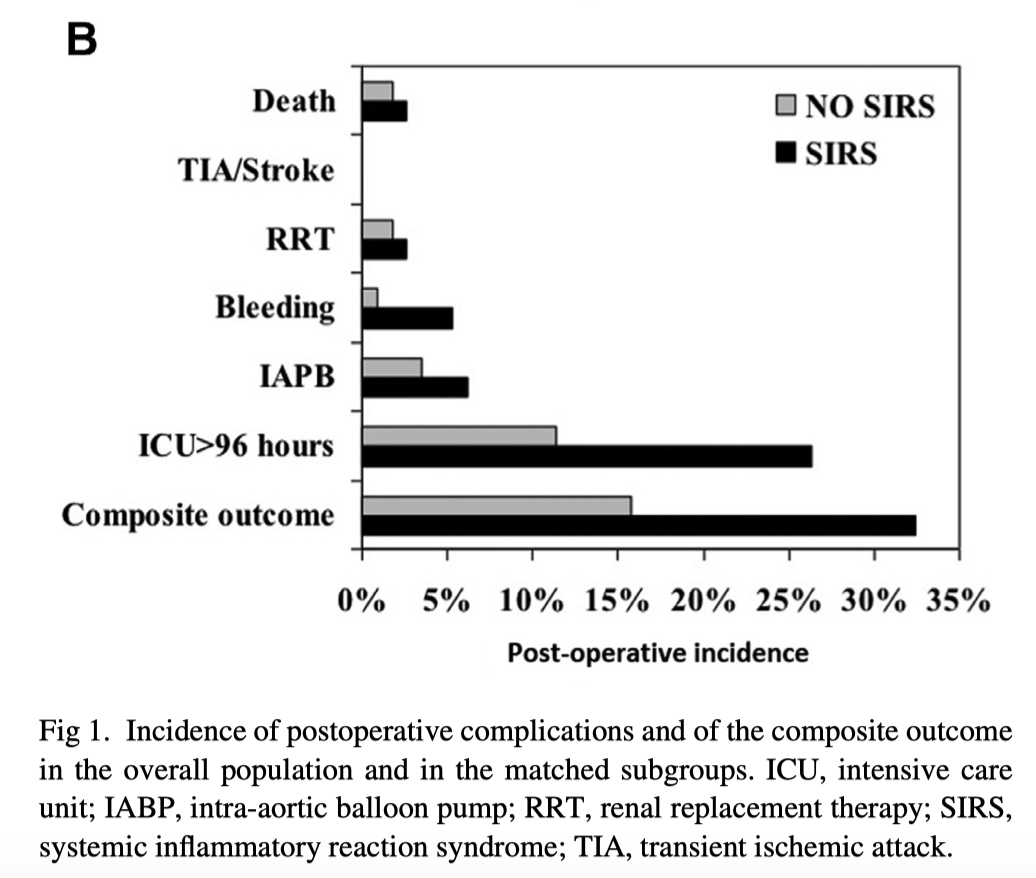
Cardiac surgery induces a systemic inflammatory reaction that has been associated with postoperative mortality and morbidity. This retrospective analysis of 502 patients aimed to assess the incidence of postop systemic inflammation after cardiac surgery. The authors concluded that the clinical signs of systemic inflammatory reaction syndrome (SIRS) were evident in a substantial percentage of patients who underwent cardiac surgery.
Postoperative atrial fibrillation (POAF) complicates 20–40% of cardiac surgical procedures and 10–20% of non-cardiac thoracic operations. Typical features include onset at 2–4 days postoperatively with a short, self-limited time course. Mechanisms likely include intraoperative and postoperative phenomena, such as inflammation, sympathetic activation and cardiac ischaemia, that combine to trigger atrial fibrillation, often in the presence of pre-existing factors. β-Blocker prophylaxis is the best-established preventive therapy and should be instituted preoperatively unless contraindicated. When POAF occurs, rate control usually suffices, and routine rhythm control is usually unnecessary.










