Welcome to the monthly SHDA Research Update. Our specialists have selected 3 seminal papers that have been recently published in each speciality (Cardiology, Cardiac Surgery, Cardiac Imaging, Perioperative Medicine).
Summarised by Sarah Catchpoole
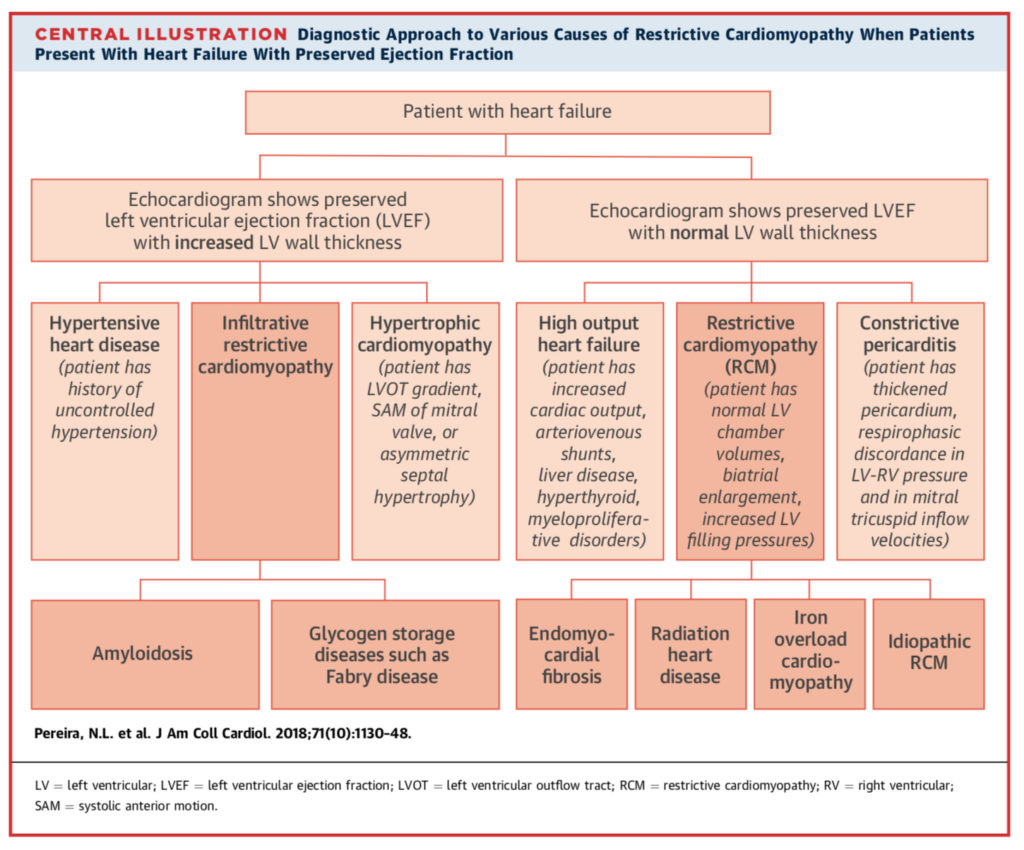
Highly recommended reading this month for all clinicians, this two part series provides a succinct revision of the restrictive and infiltrative cardiomyopathies and their causes, clinical features, diagnosis, treatment, and prognosis. Part 1 covers idiopathic restrictive cardiomyopathies and storage disorders, followed by an in depth section on cardiac amyloidosis. Part 2 reviews endomyocardial fibrosis, radiation induced, iron overload, and finally infiltrative cardiomyopathies, in particular sarcoidosis.
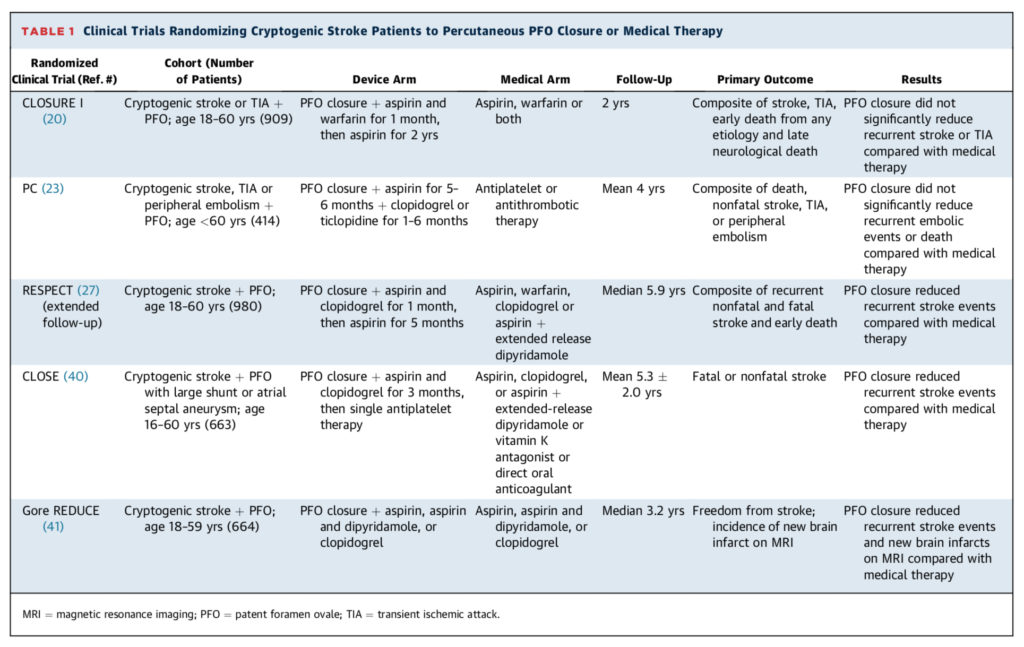
Mojadidi MK, et al. Cryptogenic Stroke and Patent Foramen Ovale. J Am Coll Cardiol. 2018 Mar 6
The prevalence of patent foramen ovale (PFO) in patients with cryptogenic stroke is 40-50% compared to 20-25% in the general population. Contrary to earlier findings, this new focused meta-analysis of all 5 randomized clinical trials (n=3440) conducted to date has found PFO closure does significantly reduce the risk of recurrent stroke, without any increase in major adverse events (2.0% vs. 4.5% with medical therapy, RR 0.42, 95% CI 0.20-0.91, p=0.027). However, PFO closure was associated with increased risk of atrial fibrillation across all trials (4.0% vs 0.7%, RR 4.55, p < 0.01), but not for all devices (RR 2.10 for the PFO occluder of PC and RESPECT, vs. RR of 7.92, 5.43, and 14.66 for the remaining devices).The authors conclude by suggesting PFO closure is beneficial, safe, and may even merit evaluation for primary prevention of stroke in high-risk persons.
Noncompaction cardiomyopathy (NCCM), formerly known as “spongy heart”, is characterised by excessive trabeculations of the left ventricle. It is associated with several genes of autosomal dominant inheritance, but appears to arise sporadically in approximately 50% of cases. This multicentre study from the Netherlands has confirmed NCCM is a heterogenous condition, and suggests genetic stratification could be used to guide clinical care. In a retrospective cohort of 327 unrelated patients, allocation into genetic, probably genetic and sporadic categories predicted age at diagnosis, left ventricular (LV) function, and final risk of major adverse cardiac events MACE). Genetic cases were more likely to have LV dysfunction and MACE, and more common in children; inversely, sporadic cases were more common in adults and less likely to have MACE.
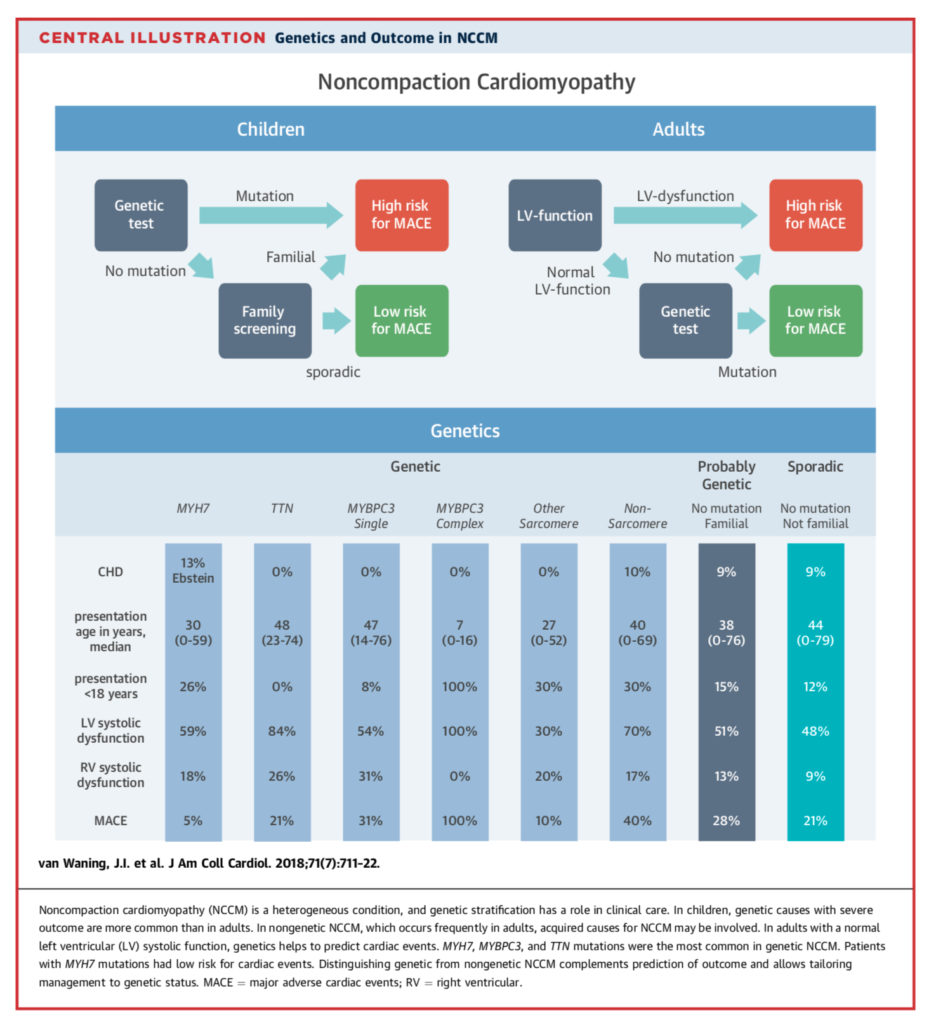
Summarised by Andrew Haymet
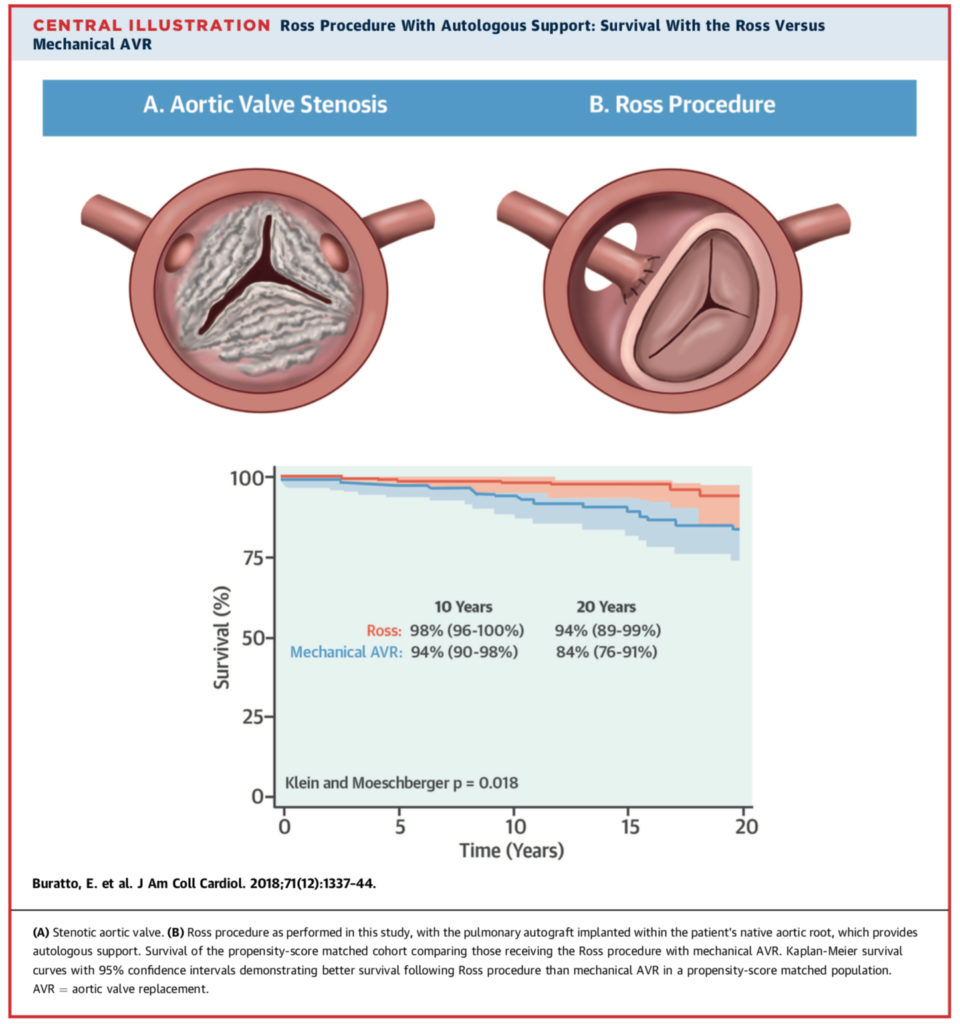
Whether or not the Ross procedure offers superior survival compared with mechanical aortic valve replacement is unclear. This Australian, propensity-score matched study compared 392 Ross procedures performed between 1992 and 2016 with 1,928 isolated mechanical AVRs performed during the same time period. Thirty-day mortality was similar (Ross, 0.3%; mechanical, 0.8%; p = 0.5). Ross procedure patients experienced superior unadjusted long-term survival at 20 years (Ross, 95%; mechanical, 68%; p < 0.001). Multivariable analysis showed the Ross procedure to be associated with a reduced risk of late mortality (hazard ratio: 0.34; 95% confidence internal: 0.17 to 0.67; p < 0.001). The authors concluded that the Ross procedure was associated with better long term survival compared with mechanical AVR, and should be considered in younger patients at experienced centres.
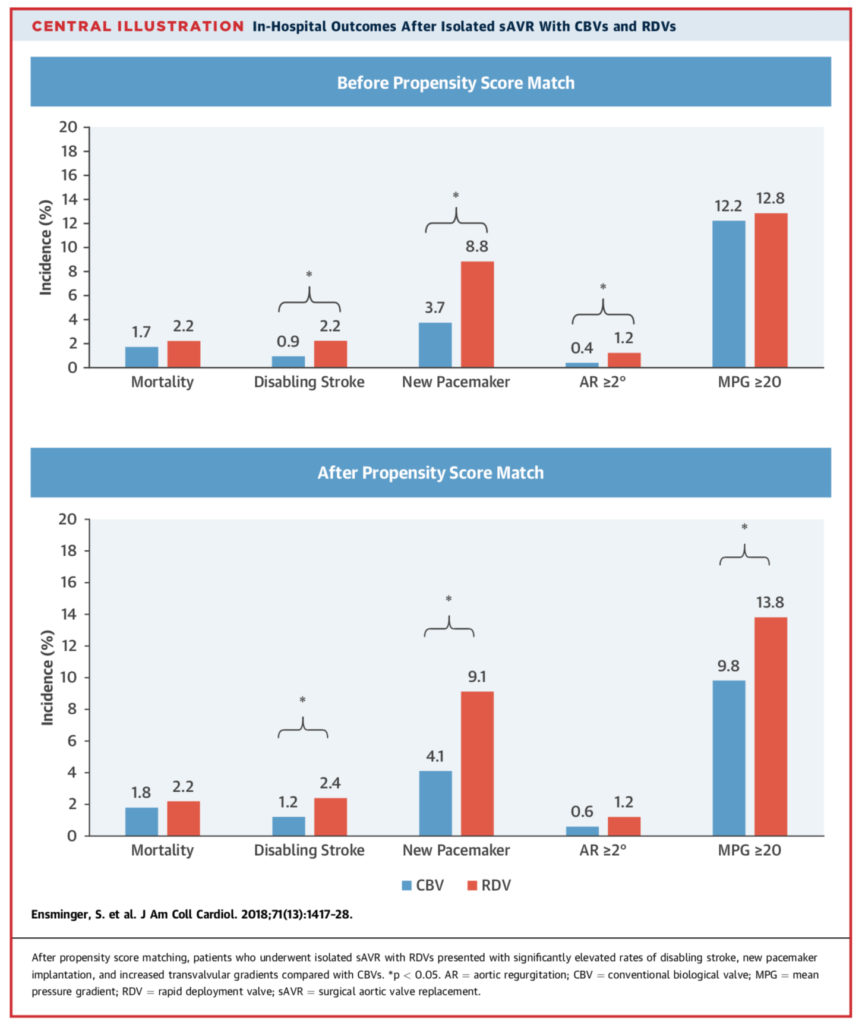
Whilst surgical aortic valve replacement (SAVR) using conventional biological valves (CBVs) is the standard of care for treatment of older patients with aortic valve disease, rapid deployment valves (RDVs) have been recently introduced. This study reported the outcomes of 22,062 patients who underwent CBV or RDV between 2011 and 2015. Patients treated with an RDV presented with significantly reduced procedure, cardiopulmonary bypass, and aortic cross clamp times, but showed significantly higher rates of pacemaker implantation (3.7%vs. 8.8%; p < 0.001) and disabling stroke (0.9%vs. 2.2%; p < 0.001). In-hospital mortality was similar (1.7% vs. 2.2%; p = 0.22). The authors concluded that in this large, all-comers database, the incidence of pacemaker implantation and disabling stroke was higher with RDVs, with no beneficial effect on mortality.
Summarised by Sarah Catchpoole
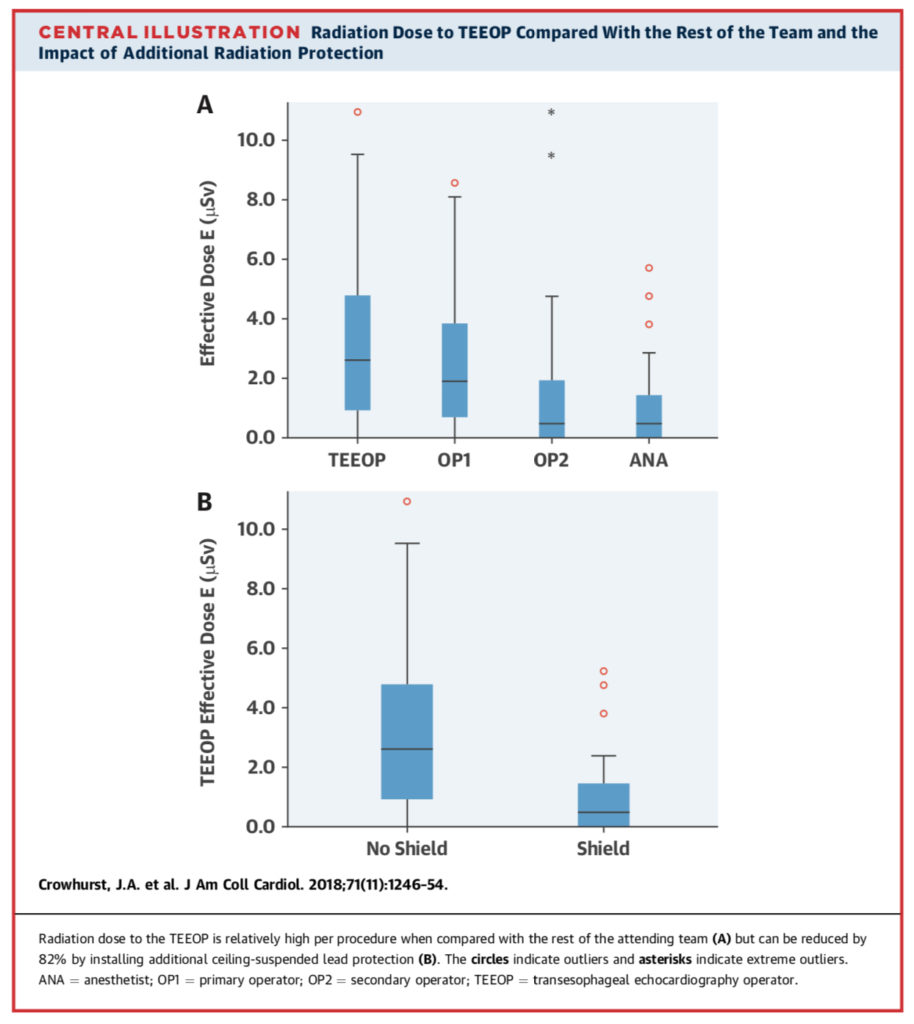
Percutaneous, fluoroscopically guided procedures are becoming an increasingly popular alternative to open surgery in many specialty fields, including cardiology. However, most studies have focused on radiation exposure and personal protection for primary proceduralists (OP1), while transoesopheageal echocardiography operators (TEEOP) are less well studied. In this single centre observational study, operating room staff wore instantly downloadable dosimeters over a period of a year. Across 98 initial procedures, there was no significant difference in radiation effective dose between TEEOP and OP1 (p=0.101), but there was significantly increased radiation effective dose compared to anaesthetists and secondary proceduralists (p<0.001, for both). After installation of additional TEEOP shielding for a further 50 procedures, radiation effective dose was reduced by 81.7% (p<0.001), with no significant change for other operating room staff.
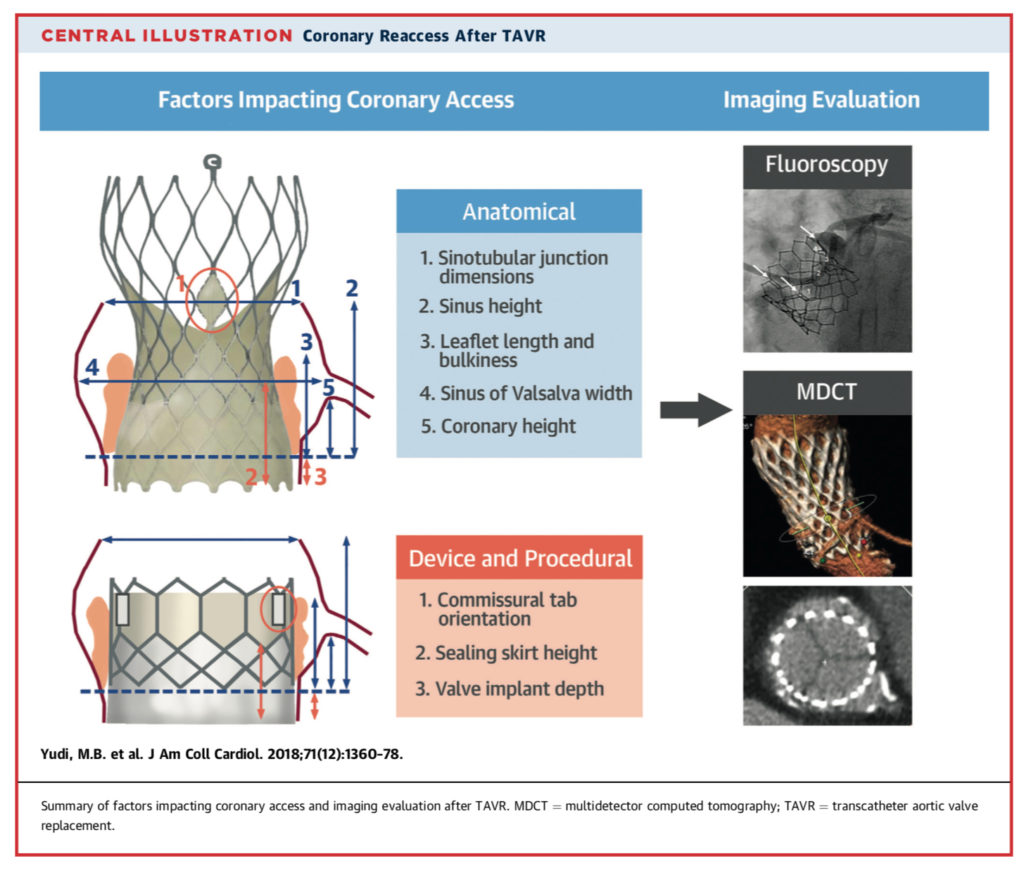
Transcatheter aortic valve replacement (TAVR) is becoming increasingly popular in intermediate and high risk patients, in whom ischaemic heart disease is common. By necessity, the devices are implanted within the proximity of the coronary ostia. However, the feasibility and difficulty of coronary angiography and percutaneous coronary interventions (PCI) after TAVR is not well studied. This narrative review collates operator experiences from available feasibility studies in the literature with greater than 5 patients. Coronary angiography and PCI appears to be most difficult in patients with balloon expandable valves; while feasible, there are reports of difficult engagement, need to use extra guide support or catheters, and even one case of a patient death secondary to a backup catheter becoming caught on a stent frame. The review goes on to discuss the biomechanics and positioning of individual TAVR devices, and propose algorithms to aid clinicians when troubleshooting in the procedural setting.
Summarised by Andrew Haymet
Enhanced recovery after cardiac surgery (ERAS) pathways have not been reported in cardiac surgery. This randomized clinical trial randomly assigned 226 patients undergoing valvular surgery to either the ERAS pathway or a routine control group. Postoperative time to readiness for discharge was significantly shorter in the ERAS group (6.0 (2.0 ~ 14.0) days) than the control group (7.0 (4.0 ~ 16.0) days, P = 0.01), and the duration of ICU stay and duration of mechanical ventilation were significantly shorter in the ERAS group (20.9 (13.5 ~ 69.3) h, 7.2 (0.0 ~ 22.3) h, respectively) than the control group (22.0 (13.4 ~ 212.3) h, P = 0.001; 8.8 (3.7 ~ 44.9) h, respectively; P < 0.0001). The authors concluded that ERAS pathways reduce the length of ICU and hospital stay, postoperative complications, and cost for patients undergoing cardiac surgery.

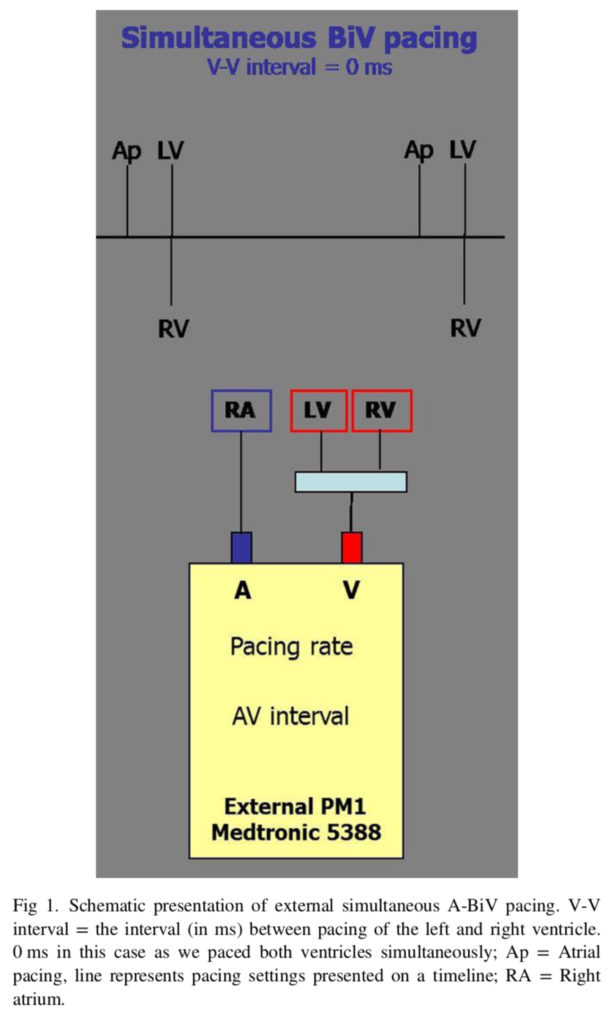
Patients with poor left ventricular function undergoing cardiac surgery have a greater chance of difficult weaning from cardiopulmonary bypass (CPB) and a poorer clinical outcome. Interventricular dyssynchrony, paradoxical septal motion, and even temporary bundle-branch block may be observed post-weaning. This prospective single centre study of 17 patients compared the effects of right ventricular (A-RV) and biventricular (A-BiV) pacing on these parameters. A-BiV pacing compared with A-RV pacing demonstrated higher arterial dP/dt values (846 +/- 646 mmHg/s vs800 +/- 587 mmHg/s, p = 0.023) and higher MAP values (77 +/- 19 mmHg vs71 +/- 18 mmHg, p = 0.036). The authors concluded that in patients with preoperative decreased left ventricular function undergoing coronary artery bypass grafting, A-BiV pacing improved the arterial dP/dt max and MAP in patients with both normal and prolonged QRS duration compared with standard A-RV pacing. Additionally, arterial dP/dt and MAP can be used to evaluate the effect of intraoperative pacing.